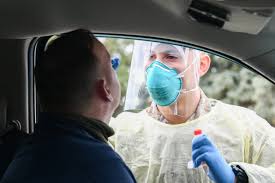
An increase in turnaround time for COVID-19 test results in pockets across the state and a decline in overall testing are due to a stressed supply chain, according to state health leaders.
In urban and rural parts of Wisconsin, a shortage in testing supplies — both the kits to collect a sample and the reagents necessary to produce a result — “continues to be a concern and it continues to be sporadic across the state,” Wisconsin Hospital Association CEO Eric Borgerding told a Wisconsin Manufacturers & Commerce briefing.
He attributes shortages to the sheer volume of people now being tested in the state. That stresses the supply chain and could affect community testing done in schools or by hospitals, drive-thru testing sites operated by the National Guard, or testing done by employers.
“The ability to continue doing that at the level we’ve been doing it is going to be really stressed because the supplies are consistently not there,” he said.
Borgerding added that health systems have had to pull back from community testing because they needed the supplies to deliver health care. DHS also expressed concern last week about testing supplies from the federal government being steered away from Wisconsin to other states.
“The bottom line is we’re nowhere near out of the woods on testing, and my concern is that if we have sort of an unbridled testing strategy, which I think is the ideal. But I don’t know if anyone, anywhere, anytime getting tested can be sustained and supported by our supply chain.”
State Health Officer Stephanie Smiley told reporters in a DHS briefing that the state is trying to diversify labs that use the PCR test — “the standard” — and procure PCR tests to keep testing supplies available in Wisconsin.
“We are actively trying to increase the capacity in Wisconsin in light of what we’re anticipating will be additional demand,” she said. “We know that we won’t be in a situation in the state or nationwide where we’re going to be able to keep up with that demand just because of where we are in terms of supply.”
Dr. Clyde Chumbley, CEO of the Wisconsin Medical Society, said in the WMC webinar that with testing supply shortages happening before flu season, the best strategy might be to only test symptomatic individuals or those exposed to the virus. Similar testing restrictions were in place when Wisconsin had low testing capacity earlier in the pandemic.
“I think we’re going to have to ask the public to step up again and think hard about when they actually need a test,” Chumbley said.
Smiley also said the state may have to develop a framework to prioritize tests if demand outruns capacity.
Chumbley said one solution might be the CDC’s recent approval of pool testing. Pool testing is when a group of people are tested and if the batch is negative, that means they are all negative. If the tests are positive, then everyone in the group would get a test to narrow down who has the virus.
There are currently no labs in Wisconsin doing pool testing, DiSalvo said, adding that it’s up to each laboratory to pursue FDA approval to do those tests in their labs.
Another positive development is the reverse transcription loop-mediated isothermal amplification (RT-LAMP) test being developed at UW-Madison and other universities.
The test, which uses saliva, also uses different chemicals that the other COVID-19 tests, which could take pressure off the current supply chain, said Chumbley. It takes up to 60 minutes to get the color indicated result, and it’s 10 percent of the cost of the PCR test.
“My hope is that this will get FDA approval and can be wrapped up quickly,” he said.
“There’s other types of tests that are coming out on the market,” Smiley said. “We need to figure out the best use for these different types of tests… and how they can complement the strategy that we already have in place with the PCR tests.”
-By Stephanie Hoff
WisBusiness.com